Modern Technology in Healthcare: Innovations Transforming the Way We Heal
Introduction
The healthcare sector is experiencing a rapid and profound transformation driven by modern technology. What once relied heavily on manual interpretation, paper records, and delayed diagnostic processes now benefits from automated analysis, digital records, and precision tools. Artificial intelligence (AI), surgical robots, wearable sensors, telemedicine platforms, advanced imaging, electronic medical records (EMR), and genomics are reshaping how clinicians diagnose, treat, and monitor patients. This article explores these innovations, their real-world applications, the benefits they bring, the challenges they pose, and what the future might look like.
1. The Role of Technology in Modern Medicine
Technology in medicine does more than increase efficiency — it saves lives. Hospitals and clinics that adopt modern tools often see faster diagnoses, fewer complications, and better long-term outcomes. Healthcare technology enables:
- Faster, more accurate diagnosis: automated image analysis and lab automation reduce human error and turnaround time.
- Targeted treatments: precision medicine personalizes therapy based on genetics and biomarkers.
- Continuous monitoring: wearables and remote sensors allow ongoing observation outside of clinical settings.
- Minimally invasive procedures: robotic systems enable smaller incisions and faster recovery.
- Digital workflows: EMRs and integrated platforms reduce documentation errors and speed care coordination.
These advances collectively support a healthcare model that is proactive, personalized, and preventive rather than reactive.
2. Artificial Intelligence (AI) in Healthcare
AI and machine learning are perhaps the most visible technologies changing clinical practice. By analyzing massive datasets—imaging, genomics, electronic health records—AI models can detect subtle patterns and predict outcomes with increasing accuracy.
Major AI applications:
- Imaging analysis: AI highlights anomalies on X-rays, CTs and MRIs, often faster than a human reader.
- Early cancer detection: algorithms trained on millions of scans can flag suspicious lesions and prioritize cases.
- Clinical decision support: AI assists clinicians with drug dosing, risk stratification, and differential diagnosis.
- Operational AI: optimizes scheduling, bed allocation, and hospital supply chains.
Real-world examples include AI systems that detect diabetic retinopathy in primary care and tools that screen mammograms for early breast cancer. However, clinical validation, regulatory approval, and careful integration into workflows remain crucial for safe deployment.
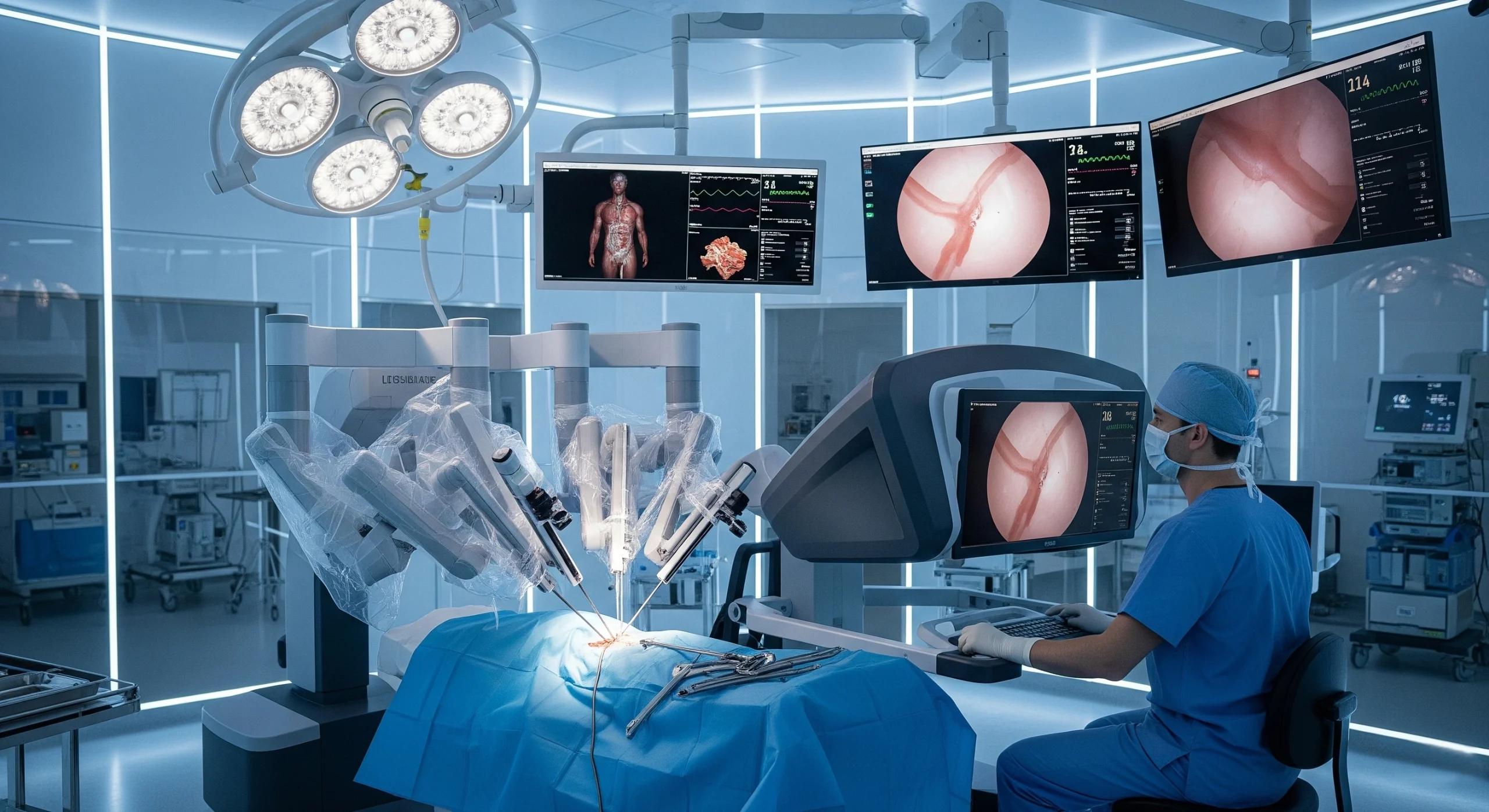
3. Medical Robotics and Precision Surgery
Robotic systems extend human capabilities in the operating room. They provide enhanced dexterity, tremor reduction, and three-dimensional visualization, allowing surgeons to perform complex procedures with smaller incisions.
Common robotic uses:
- Da Vinci Surgical System: widely used in urology, gynecology, and cardiac surgery for minimally invasive approaches.
- Orthopaedic robots: improve alignment and accuracy in joint replacements.
- Rehabilitation robots: deliver intensive, repeatable physical therapy for stroke and spinal cord injury recovery.
Robotic surgery can shorten hospital stays and reduce complications, but costs, staff training, and equitable access are ongoing challenges.
4. Wearables and Continuous Monitoring
Wearable devices—smartwatches, fitness bands, medical patches—have moved from consumer gadgets to clinical tools. They continuously collect physiological data such as heart rate, activity, sleep, SpO₂, and in some devices, ECG tracings.
Clinical benefits:
- Early detection: irregular heart rhythms or hypoxia can be identified outside the clinic.
- Chronic disease management: remote monitoring supports hypertension, diabetes, and heart failure care.
- Behavioral insights: activity and sleep data inform lifestyle interventions.
Despite their usefulness, wearables must be validated for clinical accuracy, and clinicians need infrastructure to handle the data flow and integrate it into care decisions.
5. Telemedicine and Remote Care
By enabling virtual consultations, telemedicine has expanded access to care, reduced travel burdens, and sustained healthcare delivery during crises such as the COVID-19 pandemic.
Key advantages:
- Video consultations for triage and follow-up
- Remote prescription delivery and e-referrals
- Reduced infection risk and shorter wait times
- Improved access for homebound or rural patients
Telemedicine is now embedded within national health systems, but it requires reliable connectivity, privacy safeguards, and reimbursement frameworks to be sustainable.
6. Advanced Medical Imaging
Imaging technologies continue to evolve. High-resolution MRI, fast CT scanners, portable ultrasound, and PET imaging offer more detailed, quicker, and earlier views of disease processes.
Trends and impacts:
- 3D and functional imaging: better visualization of anatomy and physiology.
- Faster scanning: reduces motion artifacts and increases throughput.
- Portable devices: bring diagnostics to bedside and remote clinics.
Combining imaging with AI can further improve sensitivity and specificity, supporting earlier intervention and better treatment planning.
7. Electronic Medical Records (EMR) and Interoperability
EMRs digitize patient information and enable secure sharing across providers, improving continuity of care. Interoperable systems facilitate referrals, longitudinal tracking, and integration with decision-support tools.
Benefits of EMR:
- Faster access to complete medical history
- Reduced transcription and medication errors
- Integration with labs, imaging, and pharmacies
- Supports population health analytics
However, EMR usability, data standardization, and clinician burnout from documentation remain important considerations.
8. Big Data and Genomics: Predictive and Precision Medicine
Genomic sequencing and big data analytics enable risk prediction and personalized therapies. By combining genetic profiles with lifestyle and environmental data, clinicians can tailor prevention and treatment strategies.
Applications:
- Genetic screening for hereditary cancer or cardiovascular risk
- Pharmacogenomics to predict drug response and avoid adverse effects
- Population-level surveillance to identify emerging health trends
Ethical issues—privacy, consent, equitable access—must be addressed as genomic medicine scales up.
9. Challenges, Risks, and Ethical Considerations
While technology offers enormous promise, it also introduces risks:
- Cost and access: high-tech solutions can widen disparities if not equitably deployed.
- Data security: health data breaches undermine trust and privacy.
- Over-reliance on automation: may reduce clinician oversight and the human touch.
- Regulatory hurdles: ensuring safety and efficacy requires robust clinical trials and oversight.
Policymakers, providers, and technology developers must collaborate to create standards, reimbursement models, and training programs that mitigate these risks.
10. Looking Ahead: The Future of Healthcare Technology
Over the next decade, we can expect rapid progress in several areas:
- Minimally invasive and even non-invasive treatments enabled by nanotechnology and focused energy delivery.
- AI-assisted personalized medicine where treatment plans evolve as new data arrives.
- Robotic and automated caregiving to address workforce shortages and support aging populations.
- Brain-computer interfaces that restore function to stroke or paralysis patients.
- Wider use of telehealth and home diagnostics making care more convenient and continuous.
The ultimate goal is a healthcare system that is predictive, preventive, personalized, and participatory—where technology empowers clinicians and patients alike.
FAQ
Can technology replace doctors?
No. Technology augments clinical decision-making and operational efficiency, but human judgment, empathy, and ethical reasoning remain irreplaceable.
Are wearables clinically reliable?
Many wearables are useful for screening and monitoring, but clinical decisions still rely on validated medical tests. Device accuracy varies by manufacturer and use case.
How can I protect my medical data?
Use providers and apps that follow recognized standards (encryption, two-factor authentication), review privacy policies, and exercise control over data sharing where possible.
Conclusion
Modern healthcare technology is reshaping medicine in fundamental ways—improving diagnosis, enabling personalized care, and extending monitoring beyond hospital walls. While challenges around cost, access, privacy, and ethics must be addressed, thoughtful deployment and regulation can ensure these innovations benefit patients globally. Embracing technology thoughtfully will help clinicians deliver safer, faster, and more compassionate care.
